New Year, New You: How an Anti-Inflammatory Coating Can Keep Joint Implants Moving Pain-Free for Longer
January 7, 2016
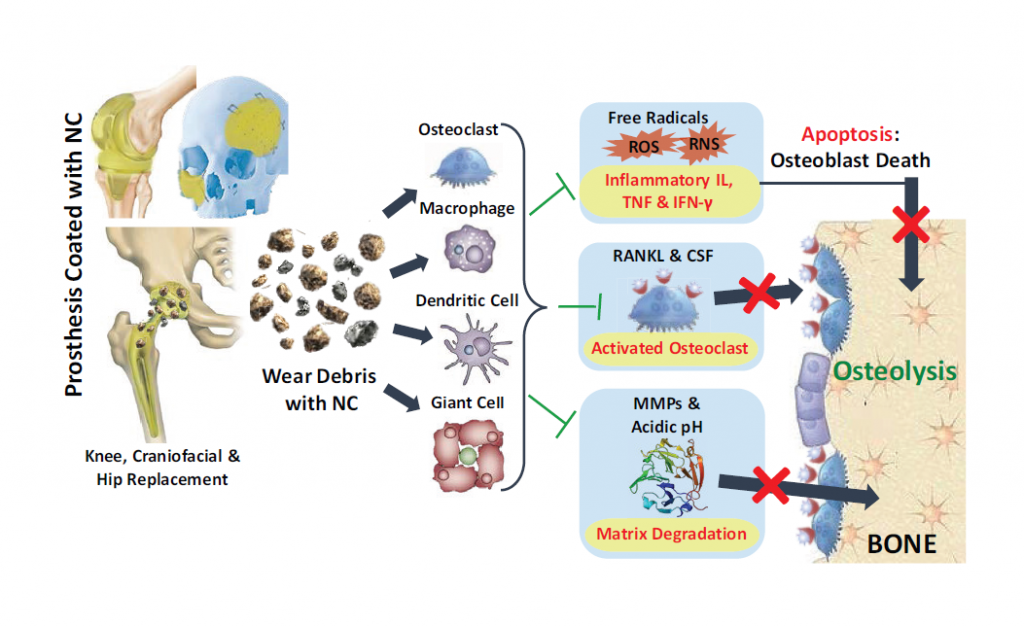
Showing the potential benefits of a prosthesis coated with the anti-inflammatory agent nanoceria
As we start the New Year, many of us will be making resolutions or goals about our physical health—promises to eat healthier and to exercise more often. For those of us who are older, ages 50 and above, we may have some specific health concerns, like chronic joint pain.
When it comes to our joints, one option that has become more and more prevalent for pain relief from conditions like arthritis is total joint replacement (TJR). Unfortunately, despite the technological advances and improvements in treating these types of conditions, TJR still remains the final treatment option in many cases. The Academy of Orthopedic Surgeons state that 90 percent of patients who undergo knee replacement surgery report a significant reduction in pain.
And the costs of these type of surgeries add up. TJR costs $10 billion annually, and the annual hospital costs associated with these procedures are projected to exceed $65 billion by 2015. Additionally, because of osteolysis (bone loss) rates of up to 40 percent, as well as chronic inflammation due to the debris of the degrading implant, 10 to 15 percent of these surgeries will fail, causing additional pain. Patients will then need revision surgeries, which cost 40 percent more than TJR surgeries. In the U.S., more than $1 billion is spent just on revision surgeries each year. Recovery time for patients is also longer with revision surgeries.
To reduce these health care costs, Sudipta Seal, Ph.D., and his team are currently developing a coating involving nanoceria (NC) for implants that would potentially reduce inflammation, promote bone integration of the implant, and thus lengthen the lifetime of the implant while reducing the number of revision surgeries.
NC has many biological applications, and within this budding technology, one of them would be as an anti-inflammatory agent with minimizing corrosion of the joint implant via restoring the redox balance in the surrounding environment. Redox is short for chemical reduction-oxidation reaction, which relates to the high number of free radicals that are created from the use of the joint replacement and the resulting inflammation and bone loss.
To give a very brief Chemistry 101 primer: a free radical is an unstable molecule that arises when weak bonds split, leaving it with unusual, unpaired electrons. This instability causes it to go around, attacking the nearest molecule so that it can steal its electrons. Then that attacked molecule becomes a free radical who then will repeat this process of theft until an antioxidant comes and restores order by giving their free electrons, neutralizing the free radical attacks that would lead to ultimate cell and tissue damage.
Another benefit of Seal’s nascent composition has to do with the roughness of the implant itself. Bone integration is a very important component of a successful TJR surgery, meaning that the patient’s bone needs to accept this foreign body as its own and does not reject it. This coating’s roughness has been reduced, so the chances of bone loss would be reduced, as well as the chance of implant failure and the subsequent revision surgery.
—
New Year, new you? For many Americans, it may mean receiving new joint replacements, and Sudipta Seal’s research may help to keep that new knee or new hip in for a lot longer, for a lot less money, and with a lot less pain. To learn more, contact Brion Berman.
Written by Deborah Beckwin.
Passive Wireless Sensors with Piezoelectric MEMS Resonators: Tiny, Mighty Machines
December 3, 2015
Sensors — devices that detect and respond to some stimulus (e.g., light, heat, motion) — are part of our everyday lives. Take a smartphone, for instance. This one small device carries a plethora of sensors that gather data for apps, such as the battery’s temperature. They use a technology called microelectromechanical systems, or MEMS.
MEMS are mini-machines, comprised of mechanical parts (e.g., levers, springs, and vibrating structures) and electrical parts (e.g., resistors, capacitors, and inductors) which measure between 1 and 100 micrometers in size. How small is that, exactly? In comparison, the diameter of a human hair is 25 micrometers and the size of a grain of salt is 100 micrometers.
These two types of parts work together to gather data and/or physically interact with the surrounding environment. These devices are currently found in items such as car airbag systems, small cameras, microphones, fitness watches like Jawbone and Fitbit, and toasters. This graphic from the MEMS Industry Group shows how we use MEMS devices on a routine basis. Yet even with the ubiquity of this technology, there are still limitations with where these sensors can be placed.
—
 One new type of sensor is a passive wireless sensor system that utilizes piezoelectric MEMS resonators created by Reza Abdolvand, Ph.D., who is also our featured researcher for the month of December. This invention is comprised of a few different parts, working in concert.
One new type of sensor is a passive wireless sensor system that utilizes piezoelectric MEMS resonators created by Reza Abdolvand, Ph.D., who is also our featured researcher for the month of December. This invention is comprised of a few different parts, working in concert.
Unlike wired sensors, which require a power source such as a battery, these new sensors scavenge energy from the signal that is transmitted from a transreceiver to a tiny antenna in the system. This makes the sensor wireless because it passively receives energy.
Piezoelectric (the prefix piezo- is Greek for “press” or “squeeze”) sensors measure changes in pressure, temperature, strain, or force by converting them into electrical charges. MEMS resonators are silicon-based, miniature structures that vibrate at high frequencies. Together, piezoelectric MEMS resonators use the best of both worlds: the electromechanical strength of the piezoelectric material and the stability of the MEMS structure are combined to create a reliable, cost-effective sensor system.
—
One of the future innovations that Abdolvand and his group is working on involves creating a smaller antenna, effectively reducing the device’s size and opening the field to new applications that otherwise wouldn’t be available or useful. This could go well beyond the sensors found in a smartphone. It may mean, for example, the ability to access biometric data, on demand, from within the human body through sensors placed just under the skin. These sensors could be placed in many areas that were previously inaccessible (e.g., the moving parts of an engine, inside rotating objects like tires). Additionally, wherever there is a wired sensor, Abdolvand’s invention could possibly replace it.
These lower cost, tiny and mighty devices can be mass-produced and can even become disposable (e.g., ensuring food safety by measuring temperature on packaged food). Soon, the future will fit on the head of a pin, offering an abundance of information to improve our everyday lives.
—
There are a myriad of possibilities with this new sensor system. If you’re interested in exploring them, contact Raju Nagaiah, Ph.D. for more information.
Movember: Bringing Awareness to Diseases like Prostate Cancer, One Mustache at a Time
November 5, 2015
 Are you starting to see your clean-shaven male friends, family members, and co-workers growing mustaches this month? It’s not just the latest fashion trend in personal grooming. You may have heard of the health awareness campaign Movember, where men grow out their mustaches to raise funds and awareness for men’s health. One of the main focal points of this campaign is prostate cancer.
Are you starting to see your clean-shaven male friends, family members, and co-workers growing mustaches this month? It’s not just the latest fashion trend in personal grooming. You may have heard of the health awareness campaign Movember, where men grow out their mustaches to raise funds and awareness for men’s health. One of the main focal points of this campaign is prostate cancer.
According to the Movember website, prostate cancer is the second most common cancer in men worldwide, with the number of cases expected to almost double to 1.7 million by 2030. It is also the most commonly diagnosed cancer and is a leading cause of death in men in developed countries. Additionally, the death rate among African American men is two times higher than any other ethnic group.
Although prostate cancer affects the lives of many men, awareness of the disease still needs to be expanded. The Mayo Clinic says in its early stages, prostate cancer may not show any signs or symptoms. However, once advanced, the following signs may be present:
- Trouble urinating
- Decreased force in the stream of urine
- Blood in the semen
- Discomfort in the pelvic area
- Bone pain
- Erectile dysfunction
—
Ratna Chakrabarti, Ph.D., cancer researcher at the Burnett School of Biomedical Sciences, was recently interviewed for our Faculty Feature. Her area of interest is prostate cancer and she explained the cycle of treatment for patients with the disease.
“Prostate cancer is a slow-growing tumor in the beginning. The way to find an aggressive tumor, or someone having prostate cancer, is very erroneous. There are not many tests available, and even with the tests that are available [prostate-specific antigen or PSA], they are not that good at predicting whether a person will develop prostate cancer or not.”
She further explained that when patients come in for treatment, there’s a waiting game: waiting for the tumor to grow.
“The first line of therapy is operation [radical prostatectomy]. This procedure takes care of the majority of the patients,” says Chakrabarti.
After surgery, the five-year survival rate is 98.9 percent. Most prostate cancer is localized, so prostate removal is an effective treatment.
“Some patients develop a recurrence of the disease. When this occurs, they are given hormone therapy to inhibit prostate cancer cell growth, but some patients do not respond. Even when some patients do respond to the therapy, after a year or so, they develop tremendous resistance,” Chakrabarti noted.
Advanced prostate cancer occurs when it metastasizes, or when cancer cells spread throughout the body. It can also develop in patients who have used hormone therapies such as Androgen Deprivation Treatment (ADT) to no avail, resulting in a more aggressive type of prostate cancer called castrate-resistant prostate cancer (CRPC). Chakrabarti’s research focuses on this type of cancer, for which there is currently no cure. For advanced prostate cancer, the five-year survival rate drops to 28 percent.
—
So, during the month of November, if you see someone you know that’s become recently mustachioed, be reminded that prostate cancer affects thousands of men across the world. But hope is on the horizon. The work of dedicated researchers such as Chakrabarti is bringing us much closer to a cure.
If you’re interested in becoming a partner to develop this technology for further use, Chakrabarti’s prognostic marker technology is available for licensing. For more information, please contact Brion Berman.